Do antidepressants really work? What are the side effects? Is all just a scam? Hopefully, this article will help answer these and many other questions about antidepressants. Additionally, it will provide you with another well-researched method for treating depression.
According to the WHO, 264 million people worldwide suffer from depression and the need for more, easily accessible treatments is obvious. Antidepressant medication is the most common treatment for depression, but many patients discontinue the treatment early because of uncomfortable side effects. Over the last ten years, a gentle form of brain stimulation (tDCS) has become an increasingly popular alternative to antidepressants, mostly because of its milder side effects. In this article, you’ll find an evidence-based guide to antidepressants, tDCS and what happens when you combine the two. We’ll finish with a summarizing comparison.

Do antidepressants really work?
Selective Serotonin Reuptake Inhibitors (SSRI) are a common form of antidepressant medication, prescribed to millions of people worldwide. Even though SSRI have been in use for decades, researchers still don’t know exactly why they work. But they do work. In 2018, a research team led by Professor of Psychiatry Andrea Cipriani, included 522 trials and 116 477 participants in a meta-analysis exploring the effectiveness of 21 antidepressant medications. The researchers found that all antidepressants were more effective than placebo in depressed adults. Here are the most effective ones:
- Amitriptyline
- Mirtazapine
- Venlafaxine
- Paroxetine (Paxil)
- Sertraline (Zoloft)
- Fluoxetine (Prozac)
- Citalopram (Celexa)
- Reboxetine

In an interview with the Guardian, Professor Cipriani states that around 60% of depressed patients notice a 50% reduction in their symptoms after two months using antidepressant medication. These numbers are similar to the success rates of psychotherapy, such as CBT. He also points out that any of the antidepressants on the list can be useful. A meta-analysis can only study the antidepressants’ effects on groups of people, it can’t show which drug would be most likely to work for any one individual. That’s why doctors need more than one medication to choose from when prescribing antidepressants. If one doesn’t work, maybe another one will. Additionally, doctors need to take side effects into account. In Cipriani’s study, three antidepressant drugs stood out as both effective and well tolerated by patients:
- Agomelatine
- Escitalopram
- Vortioxetine
As you see, the most effective drugs are not always the doctor’s first choice. This is why it takes time to find the right antidepressant. Doctors don’t know beforehand which antidepressant will be most effective for the individual patient or which one will give tolerable side effects. This brings us to some of the biggest problems with antidepressant medication.
“About 80% of people stop antidepressants within a month”
What is the biggest problem with antidepressant medication?
So far, we’ve concluded that around 60% of people taking antidepressants notice a significant reduction in their depressive symptoms. This means that 40% may not be helped, though that is not the biggest problem with the antidepressant drugs. It turns out that most people stop their drug treatment early, usually because of uncomfortable side effects. The following list includes common side effects from antidepressants:
- Insomnia
- Sleepiness during the day
- Restlessness
- Weight gain
- Diminished sexual interest, desire, performance and satisfaction
- Headaches
- Joint pain and muscle pain
- Muscle spasms/twitching
- Dry mouth
- Profuse sweating
- Skin rashes
- Dizziness
- Nausea
- An upset stomach
- Constipation
- Diarrhea
Taking antidepressants is generally safe, but as you can see from the list above, not always pleasant. In 2013, a research team from the Netherlands analyzed 927 cases of antidepressant use in a naturalistic study. The researchers concluded that side effects from antidepressants persist during long-term use and that a higher dose of medication are associated with more severe side effects.
Read more about the side effects of antidepressants here: What are the side effects of antidepressants? – Learn about side effects, tolerance and withdrawal

Mixing antidepressants with other drugs
If you’re already on another form of medication and thinking about taking antidepressants, there is reason to be very cautious. Even though doctors usually prescribe medications with well-known side effect profiles, it’s very difficult for medical professionals to predict how two different drugs will interact with each other. Sometimes, two drugs in combination create unexpected side effects. For example, mixing Pravastatin or Pravachol (a drug for high cholesterol) and Paroxetine or Paxil (an antidepressant) creates an unexpected and unhealthy spike in glucose levels. High glucose levels are associated with an increased risk for diabetes and, over the long term, associated with damage to organs and tissues. Researcher Russ Altman, who is studying unexpected drug interactions, can tell you more about it in his TED-talk.
According to Harvard Health Publishing, antidepressants should not be mixed with St. John’s wort (a herbal remedy), monoamine oxidase inhibitors, such as Phenelzine (Nardil) and Clomipramine (Anafranil) or lithium (a common treatment for Bipolar disorder).
Antidepressant discontinuation syndrome
Lowering the dose of an antidepressant medication or stopping the treatment too abruptly, may result in what researchers call “Antidepressant discontinuation syndrome”. According to the article written by researchers M. Gabriel and V. Sharma in 2017, the syndrome may result in a variety of symptoms, such as:
- Flu-like symptoms (lethargy, fatigue, headache, achiness, sweating)
- Insomnia (with vivid dreams or nightmares)
- Nausea (sometimes vomiting)
- Imbalance (dizziness, vertigo, light-headedness)
- Sensory disturbances (“burning,” “tingling,” “electric-like” or “shock-like” sensations)
- Hyperarousal (anxiety, irritability, agitation, aggression, mania, jerkiness)
The Antidepressant discontinuation syndrome is common. According to Gabriel & Sharma, around 20% of patients are affected by it after significantly lowering a dose of an antidepressant or after stopping the treatment abruptly.
Can brain stimulation be an alternative to antidepressants?
So far we’ve concluded that antidepressants can be effective for treating depression. At the same time, the pills come with uncomfortable side effects and sometimes unexpected problems when mixed with other forms of medications. In the last 10 years, researchers have shown a lot of interest in different types of brain stimulation as alternatives to antidepressants.
Transcranial Direct Current Stimulation (tDCS) is a form of gentle brain stimulation that uses a low-strength electric current to help activate the brain cells in an area in the front section of the brain. tDCS should not be confused with electroconvulsive therapy (ECT). The tDCS current (0,5-2 mA) is 400 times weaker and is delivered through two electrodes, placed on the scalp.
A brain stimulation session with tDCS is usually 30 minutes and can be administered at home with a tDCS headset.
So, if you’re not interested in antidepressants, could you use tDCS to recover from depression? The answer is yes. Recent research has shown that tDCS can be an effective alternative to antidepressants, especially if you’re currently taking other forms of medications or if you don’t want to deal with severe and uncomfortable side effects. In 2016, Marom Bikson and colleagues studied over 33.200 tDCS sessions in a meta-analysis with over 1000 participants. They found tDCS to be a safe treatment that has never been associated with serious adverse events. Side effects from tDCS are fewer and milder than those from antidepressant medication. Side effects from tDCS include:
- Mild stinging or burning sensations under the electrodes during stimulation
- Skin redness
- Mild headaches that pass after 30 minutes

How effective is tDCS?
Some studies show that the effectiveness of tDCS is comparable to antidepressant medication and some studies show that medication is more effective than tDCS. The research studies agree that treating depression with tDCS is significantly more effective than placebo.
“…we found tDCS to be efficacious across outcomes in both pairwise and network meta-analyses.”
“Active tDCS was significantly superior to sham in all outcomes.”
One of the largest tDCS studies showed that 41% of depressed people noticed a 50% reduction of their symptoms within 6 weeks and that 24% fully recovered from depression with tDCS treatment.
How does tDCS work?
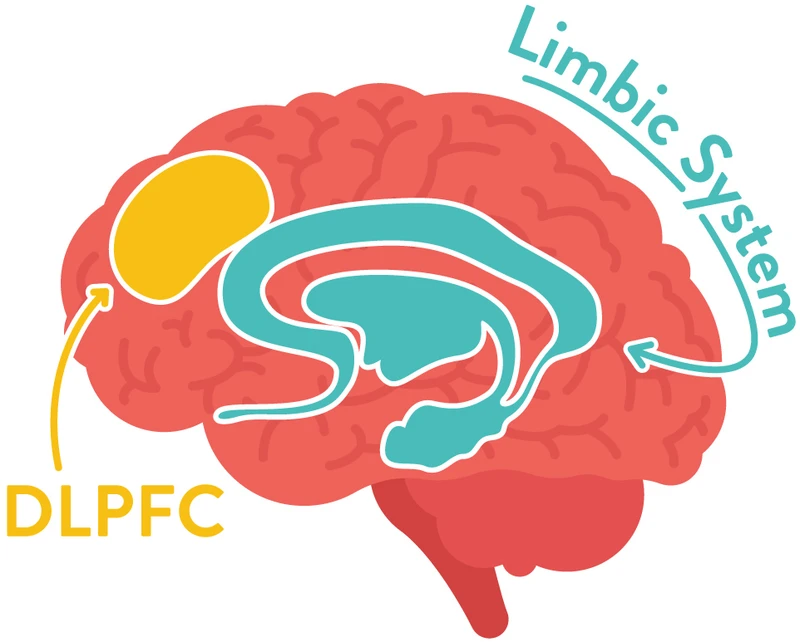
As with antidepressant medication, researchers can’t know for sure why tDCS works, but the likely hypothesis is that the treatment helps activate the brain cells in a specific brain area responsible for mood regulation. Brain images of depressed patients show that depression is associated with lowered activity in an area in the front of the brain, called the dorsolateral prefrontal cortex (DLPFC). When the activity in the DLPFC is unbalanced, it can lead to depressive behaviours, such as appetite changes, sleep disturbance and low energy levels.
When treating depression, the tDCS electrodes are placed high up on the forehead to help target this area. tDCS sends gentle electrical signals to the DLPFC, increasing blood flow and metabolism. This way, the brain cells become more easily activated, brain function is restored and the depressive symptoms decrease.
Where can I get tDCS?
Flow Neuroscience has developed the first CE-marked and medically approved tDCS device for home use. It can be used by anyone who is over 18 years of age and has a diagnosis of depression (Major Depressive Disorder). You can order it here. The tDCS device is Bluetooth controlled and managed via the Flow Depression app.
What happens when you combine antidepressants with tDCS?
All treatments for depression have one thing in common, they work for some people and for some they don’t work at all. Unfortunately, there is no depression treatment that helps everyone. The good news is that you can combine different types of treatments and increase your chances of recovering from depression. Several research studies have found that combining antidepressants and tDCS gives a more effective treatment than using either of the two separately. In 2013, Dr. Andre Brunoni and colleagues studied the effects of Sertraline (a common antidepressant), tDCS and placebo (sham treatment) in 120 research participants with moderate to severe depression. They found that the combined treatment using both tDCS and antidepressant medication was significantly more effective than tDCS only or antidepressants only. The combined treatment was the only one that resulted in significant improvements after only two weeks.
“In MDD, the combination of tDCS and sertraline increases the efficacy of each treatment. The efficacy and safety of tDCS and sertraline did not differ.”
The researchers point out that depression is associated with changed activity in the DLPFC (read more about this brain area under the headline How does tDCS work?), but also with dysfunction in the limbic system of the brain. They hypothesized that tDCS improves the function of the DLPFC and that antidepressants improve the function of the limbic system. That could explain why participants who were given both treatments felt significantly better than the rest; the combined treatment improved two different areas of the brain simultaneously.
Comparing antidepressants and tDCS - a brief overview
EFFECTIVENESS
Both treatments are significantly more effective than placebo. Some studies suggest that antidepressants and tDCS are equally effective for treating depression, while other studies suggest that antidepressants are more effective. You get the best results when combining tDCS and antidepressant medication.
SIDE EFFECTS
- Antidepressants: Common side effects from antidepressants include insomnia, sleepiness during the day, restlessness, weight gain, diminished sexual interest, desire, performance and satisfaction, headaches, joint pain and muscle pain, muscle spasms/twitching, dry mouth, profuse sweating, skin rashes, dizziness, nausea, an upset stomach, constipation and diarrhea. In general, the antidepressant medications called SSRI give milder side effects than other forms of antidepressants.
There is reason to be very cautious about mixing antidepressants with other drugs. It can be difficult for medical professionals to predict how two different drugs will interact with each other. - tDCS: Common side effects from tDCS include mild stinging or burning sensations under the electrodes during stimulation, skin redness and mild headaches that pass after 30 minutes.
TREATMENT PROTOCOL
- Antidepressants: A diagnosis of depression, a prescription and regular visits to your physician are required to receive treatment with antidepressant medication. It could take some time before you find the right kind of medication and the appropriate dose, but when you do, the procedure is fairly simple: swallow the pill, usually once a day. Most people notice a reduction of their symptoms within two months.
- tDCS: If you have a diagnosis of depression, you don’t need to visit a clinic to use tDCS. The treatment from Flow Neuroscience is medically approved to use at home. You can buy it online and have it delivered to your door. You’ll receive five 30-minute stimulation sessions per week, during the first three weeks. After that, there will be one or two sessions per week for as long as you like. You can resume daily activities after the brain stimulation sessions. Most people feel a reduction of their symptoms within 3-4 weeks.
If you don’t have a diagnosis, contact a medical professional for a mental health consultation. In the UK, you can reach out to the Chelsea Psychology Clinic. In Sweden, you can contact Kry.
The tDCS treatment from Flow Neuroscience
- Order the Flow headset from the webshop.
- Download the free depression app.
- In a few days, your headset will be delivered. When it arrives, unpack your headset and start the app.
- The app will show you how to put your headset on and how to start the stimulation. Just follow the instructions.
- You’ll receive 5 stimulation sessions of 30 minutes per week, during the first 3 weeks. After that, there will be 1 or 2 sessions per week for as long as you like.
- Most people feel a reduction of their depressive symptoms after 3-4 weeks.
Thanks for your attention!


